Knee Effusion on MRI: Fluid, Swelling, and Injury
Learn what knee effusion on MRI means, why fluid builds up, and how it relates to meniscus, ligament, ACL graft, and Baker’s cyst findings.
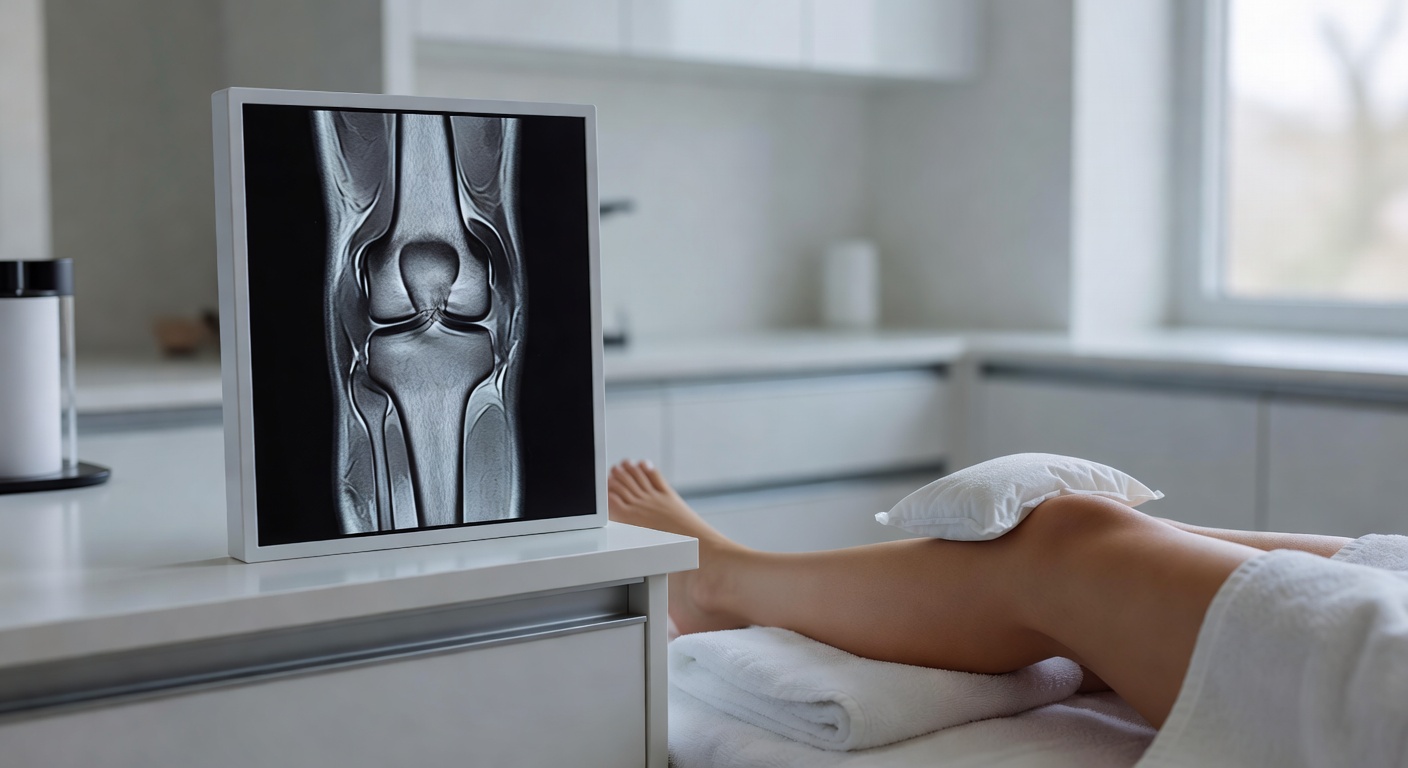
What does knee effusion on MRI mean?
A knee effusion means there is more fluid than usual inside the knee joint. On MRI, this fluid often looks bright on fluid-sensitive images and may collect above the kneecap, along the sides of the joint, or behind the knee. Radiology reports may describe it as a small, moderate, or large effusion.
A little joint fluid is normal. It helps the knee move smoothly. Extra fluid is the knee’s response to irritation, injury, inflammation, arthritis, infection, or recent surgery. In other words, effusion is not a diagnosis by itself. It is a clue that something has irritated the joint.
This article is for general education only. It cannot diagnose the cause of your knee swelling, and it does not replace a medical exam or an official radiology report.
Why does the knee make extra fluid?
The inside of the knee is lined by a thin tissue called the synovium. This lining makes joint fluid. When the knee is injured or inflamed, the synovium can become more active and produce extra fluid.
Common reasons for knee effusion include:
- Recent injury: A twist, fall, sports injury, or direct blow can irritate the joint.
- Meniscus injury: A tear in the shock-absorbing cartilage can cause swelling, pain, catching, or locking.
- Ligament sprain: Injuries to the MCL, ACL, PCL, or other stabilizing structures can lead to fluid and soft-tissue swelling.
- Bone bruise: A strong impact can injure the bone marrow without causing a visible fracture.
- Arthritis or cartilage wear: Roughened cartilage can irritate the joint lining.
- After surgery: Prior ACL reconstruction or other procedures can leave postoperative changes, and the knee may produce fluid if irritated.
- Inflammatory or infectious causes: Less commonly, swelling can be related to inflammatory joint disease or infection, which needs prompt medical evaluation.
How swelling can feel in daily life
Knee fluid can cause symptoms even when the underlying injury is small. The joint capsule stretches as fluid builds up, which may create pressure, tightness, or aching. Some people notice that the knee feels puffy above the kneecap or stiff when bending.
Effusion may be linked with:
- Pain: Especially with stairs, squatting, twisting, or sports.
- Stiffness: The knee may not bend or straighten fully.
- Locking or catching: This can happen with some meniscus tears or loose fragments, though not every click is serious.
- Instability: A feeling that the knee may give way can occur with ligament injury or muscle inhibition from swelling.
- Reduced confidence: Even mild swelling can make the knee feel less coordinated.
Symptoms do not always match the size of the effusion. A small effusion can be painful, while a larger one may feel mostly tight. That is why MRI findings are interpreted together with the history, physical exam, and full set of images.
Common MRI report terms explained
Synovitis
Synovitis means irritation or inflammation of the joint lining. On MRI, the report may describe thickened synovium, frond-like tissue, debris, or irregular material within the fluid. This can happen after injury, surgery, arthritis, or inflammatory conditions. Synovitis helps explain why the knee keeps making extra fluid.
Baker’s cyst
A Baker’s cyst, also called a popliteal cyst, is a pocket of fluid behind the knee. It often forms when extra joint fluid tracks backward through a small opening at the back of the joint. A small Baker’s cyst may cause no symptoms. A larger or leaking cyst can create fullness, tightness, or discomfort behind the knee and sometimes swelling down the calf.
Meniscus tear
The menisci are C-shaped pads of cartilage that help cushion and stabilize the knee. MRI reports may mention a suspected tear in the posterior horn, body, or root of the medial or lateral meniscus. Meniscus tears can be associated with joint line pain, swelling after activity, catching, or true locking. However, MRI findings must be matched to symptoms because some meniscus changes are not the main pain source.
MCL sprain
The medial collateral ligament, or MCL, supports the inner side of the knee. MRI may show edema, which means swelling in the soft tissues around the ligament. A low-grade sprain may show surrounding fluid while the ligament fibers remain continuous. More severe injuries can show partial or complete tearing. MCL injuries often follow a force that pushes the knee inward or twists it.
Bone bruise
A bone bruise is an area of bone marrow swelling, often from impact or compression during an injury. It is not the same as a displaced fracture. On MRI, bone bruises can look bright on fluid-sensitive images. They can be painful and may help explain why the knee hurts after trauma even when X-rays do not show a break.
ACL graft appears intact
After ACL reconstruction, MRI reports often describe tunnels in the thigh bone and shin bone, as well as small metal or fixation artifacts. If the report says the ACL graft appears intact, it means the reconstructed ligament fibers look continuous on the images reviewed. Sometimes the report adds that assessment is limited by artifacts or by only one MRI sequence. This means the finding is reassuring but not always final without the complete MRI study and a clinical stability exam.
Why a single MRI series may not tell the whole story
Knee MRI is usually read using several image types and planes, including sagittal, coronal, and axial views. Each view shows different structures better. For example, meniscus tears may be easier to confirm when sagittal and coronal images are reviewed together. Ligaments, cartilage, bone bruising, and postoperative ACL grafts also require a complete set of sequences.
Reports based on limited images may say that a tear, graft injury, or cartilage problem cannot be excluded. This does not mean the injury is definitely present. It means the available images are not enough to rule it out confidently.
How doctors connect MRI findings with symptoms
A knee MRI is one part of the puzzle. Clinicians usually compare the imaging with how the injury happened, where the pain is located, whether the knee feels unstable, and whether there are mechanical symptoms such as locking. They may also check range of motion, tenderness, ligament stability, and walking pattern.
For example, a suspected medial meniscus tear may matter more if there is inner joint line pain and catching. An MCL sprain may fit when pain and tenderness are on the inner side of the knee after a twisting injury. A large effusion after prior ACL surgery may lead the clinician to consider graft irritation, meniscus injury, synovitis, cartilage damage, or other causes depending on the exam.
Treatment depends on the cause, severity, timing, overall health, activity goals, and exam findings. Some knee effusions improve as the underlying irritation settles, while others need closer evaluation. Decisions about bracing, physical therapy, medications, injections, aspiration of fluid, or surgery should be made with a qualified clinician who can review the full situation.
When to talk to your doctor
Talk to a doctor or sports medicine clinician if knee swelling persists, keeps returning, follows an injury, or is linked with pain, stiffness, locking, catching, or a feeling of instability. Seek prompt medical care if the knee becomes very red or hot, swelling increases quickly, you have fever, severe pain, new calf swelling, or you cannot bear weight. This information is general education and is not a diagnosis.