Big Toe Arthritis, Bunions, and MRI Findings
Learn how MRI terms around the big toe joint may relate to pain, stiffness, swelling, bunions, and hallux rigidus.
This article is for general education only. It is not a diagnosis and cannot replace a visit with a qualified health professional who can examine your foot and review your full imaging study.
Why the big toe joint matters so much
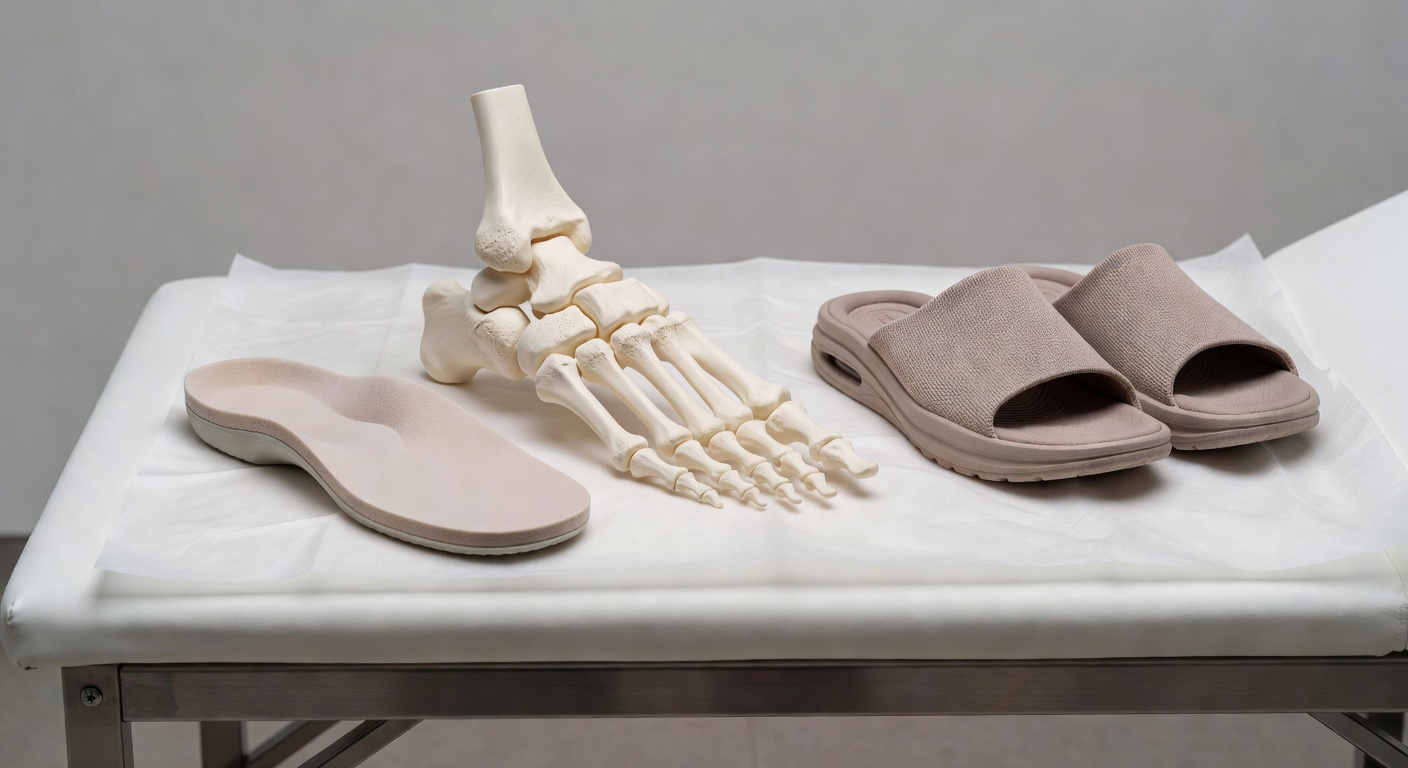
The big toe joint, also called the first metatarsophalangeal joint or first MTP joint, plays a major role in walking. Each time you step forward, this joint bends as your body rolls over the ball of the foot. If the joint is irritated, stiff, swollen, or arthritic, everyday activities such as walking, climbing stairs, kneeling, or wearing certain shoes can become painful.
Foot MRI reports often focus on this area when a person has pain near the ball of the big toe, a visible bunion, stiffness when pushing off, swelling on the inner side of the foot, or soreness under the big toe where the small sesamoid bones sit.
Imaging words such as arthritis, synovitis, bursitis, sesamoid irritation, ganglion, and hallux rigidus describe different pieces of the same neighborhood: the big toe joint and the soft tissues around it.
Common MRI terms around the big toe
First MTP arthritis
Arthritis means wear, inflammation, or damage involving a joint. On MRI, this may appear as joint space narrowing, cartilage loss, bone spurs, small cyst-like changes in the bone, bone marrow swelling, or extra joint fluid. In the big toe, arthritis can cause aching, stiffness, swelling, and pain with push-off during walking.
MRI can show inflammation and bone changes that may not be obvious on a routine exam. However, MRI findings do not always match pain perfectly. Some people have visible arthritis with mild symptoms, while others have significant pain from smaller areas of irritation.
Hallux rigidus
Hallux rigidus means a stiff big toe. It is usually related to arthritis of the first MTP joint. Hallux means big toe, and rigidus means rigid or stiff. People often notice reduced upward motion of the toe, pain when walking uphill, discomfort with running, or trouble wearing shoes that require the toe to bend.
On imaging, hallux rigidus may be described with terms such as degenerative change, osteophytes, cartilage loss, subchondral cysts, or joint space narrowing. Osteophytes are bone spurs that can form around the joint and may contribute to shoe pressure or a bump on the top of the joint.
Bunion and hallux valgus changes
A bunion is the visible bump that forms on the inner side of the big toe joint. Hallux valgus describes the alignment change in which the big toe angles toward the second toe while the first metatarsal shifts inward. Many people use the word bunion for both the bump and the overall deformity.
MRI may mention a medial prominence, soft tissue thickening, capsular irritation, or bunion-type change. The inner side of the joint may become tender because of pressure from shoes, friction, or inflammation in nearby soft tissues.
Synovitis, capsulitis, and joint fluid
The lining of a joint is called the synovium. When it becomes inflamed, the report may use the word synovitis. Capsulitis means irritation of the capsule, the soft tissue envelope around the joint. Both can lead to extra fluid in or around the joint, sometimes called an effusion.
In plain language, these terms often mean the joint is irritated. This can happen with arthritis, overuse, altered foot mechanics, injury, inflammatory arthritis, or sometimes crystal-related conditions such as gout. Imaging alone cannot determine every cause, so symptoms, exam findings, and sometimes lab tests may be needed.
Sesamoid irritation
Under the big toe joint are two small bones called sesamoids. They act like tiny pulleys for the tendons and help absorb pressure during push-off. Pain from the sesamoid area is often felt under the ball of the big toe, especially when walking, running, dancing, or standing on the forefoot.
MRI may describe sesamoiditis, sesamoid-metatarsal arthritis, bone marrow edema, or fluid around the sesamoids. These findings can overlap with big toe arthritis because the sesamoids are part of the same functional joint complex.
Bursitis and small ganglion-like fluid collections
A bursa is a small fluid-filled cushion that can form or become irritated where there is pressure or friction. Around a bunion, reports may mention adventitial bursitis, which means a pressure-related bursal sac has developed in the soft tissue. This may feel like a tender, swollen spot near the shoe line.
A ganglion is another type of fluid-filled structure that can arise from a joint or tendon sheath. On MRI it often looks bright on fluid-sensitive sequences. Small ganglion-like collections are usually described as fluid-filled, cystic, or lobulated. Whether they are painful depends on their size, location, and pressure on nearby tissues.
How MRI findings may connect with symptoms
Big toe joint findings on MRI may help explain several common symptoms:
- Pain when pushing off: arthritis, hallux rigidus, sesamoid irritation, or synovitis can make the final part of a step painful.
- Stiffness: joint space narrowing, cartilage loss, and bone spurs can reduce big toe motion.
- Swelling near the bunion: capsulitis, bursitis, synovitis, or shoe pressure may cause visible fullness.
- Pain under the big toe ball: sesamoid irritation or arthritis under the metatarsal head may be involved.
- Pressure from shoes: bunion prominence, bone spurs, or inflamed soft tissue can rub against narrow footwear.
It is important to match the MRI report with the exact painful spot. A skin marker placed during the scan can help the radiologist compare the imaging findings with the area of concern.
Why weight-bearing X-rays are sometimes mentioned
Even when an MRI has been done, a clinician may still request weight-bearing X-rays. These are X-rays taken while standing. They show how the bones line up under real body weight, which is especially useful for bunions, hallux valgus, flatfoot mechanics, and arthritis severity.
MRI is excellent for soft tissues, bone marrow swelling, joint fluid, tendons, and small cyst-like fluid collections. Weight-bearing X-rays are often better for measuring alignment, seeing the joint space under load, and planning treatment if a bunion or hallux rigidus is significant. The two tests answer different questions.
Non-surgical options often discussed
Treatment depends on the cause of symptoms, the exam, activity goals, and the full imaging report. Common conservative options that clinicians may discuss include:
- Footwear changes: shoes with a wide toe box may reduce bunion pressure. A stiffer sole or rocker-bottom sole may reduce painful big toe bending.
- Activity modification: temporarily reducing high-impact activity, hill walking, or movements that force the toe upward may help calm irritation.
- Orthotics or inserts: custom or over-the-counter supports may reduce pressure through the first MTP joint or sesamoids.
- Padding and spacers: bunion pads or toe spacers may reduce rubbing for some people, though they do not reverse arthritis.
- Physical therapy: mobility, calf flexibility, gait mechanics, and strengthening may be addressed when appropriate.
- Anti-inflammatory strategies: clinicians may discuss medicines or injections in selected situations, depending on the diagnosis and medical history.
Some people with ongoing pain, severe stiffness, progressive deformity, or difficulty with daily activities may be referred to a foot and ankle specialist to discuss additional options. Surgery is not based on MRI alone; it depends on symptoms, alignment, X-rays, exam findings, and personal goals.
Reading an MRI report with the right expectations
MRI reports can sound alarming because they list many detailed findings. Words like edema, cystic change, degeneration, and effusion describe what is seen on the images, not necessarily how serious the problem is for a particular person. Also, a limited image set or single MRI sequence may not be enough for a complete assessment. A final radiology report usually considers multiple planes and sequences.
The most helpful question is not only what does the MRI show, but does this finding match my pain pattern, exam, and walking limitations?
When to talk to your doctor
Talk with your doctor, orthopedist, podiatrist, or foot and ankle specialist if big toe pain persists, limits walking, causes increasing stiffness, or makes it difficult to wear shoes. Seek prompt medical attention for rapidly worsening pain, inability to bear weight, spreading redness, warmth, fever, a wound, or sudden major swelling. This information is general education and should not be used to diagnose or treat your own condition without professional care.